Caregiving is an activity rooted in compassion, but it also comes with real legal and logistical responsibility. Whether you are caring for an aging parent,…


Caregiving is an activity rooted in compassion, but it also comes with real legal and logistical responsibility. Whether you are caring for an aging parent,…

Last week, I gave my students at Shenandoah University an assignment: take a “principle” listed on the United Nations Principles for Older Persons webpage and…

Family caregiving—whether it is elder care or caring for an otherwise disabled individual—involves offering physical, emotional, and logistical support to a loved one who requires…
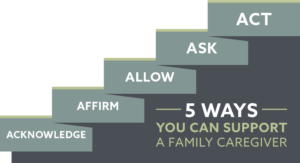
It’s not uncommon for family caregivers to feel like they are invisible. In the family caregiver role, they continually serve their loved one. The needs…

As I meet caregivers across the country, they tell me, time and again, how their lives have changed. Many changes involve the tasks of care…
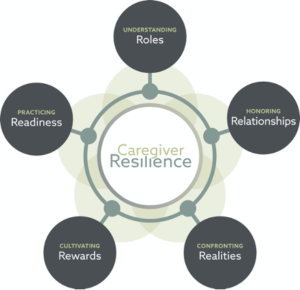
When I first introduced the model of caregiver resilience, I explained that this is a learning model. In today’s installment of the series of blog…