I’ve recently worked with human resource (HR) leaders from a range of organizations to strengthen their internal support for employees with family caregiving responsibilities at…


I’ve recently worked with human resource (HR) leaders from a range of organizations to strengthen their internal support for employees with family caregiving responsibilities at…
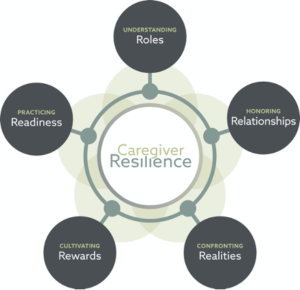
Resilience is the ability to adapt to difficult situations. Resilient caregivers find the strength to continue to help others, even in the face of adversity.…

Caregiving consultant and healthcare keynote speaker Dr. Aaron Blight takes time to post topics and answer questions on Quora about caregiving organizational development, senior care,…

Today I had the privilege of delivering the keynote address at Beloved Foundation’s REACH Oncology Symposium at the University of California Riverside. Attendees were from…